Innovations in Pharmacy Training and Sustainable Practice to Advance Patient Care: Proceedings of a Workshop (2025)
Chapter: 5 Next-Gen Education and Training Programs
5
Next-Gen Education and Training Programs
KEY POINTS*
- While pharmacy has changed greatly over the years, it is important to continue to adapt and evolve. (DiPiro)
- Expose learners to high-quality interprofessional practice, community-connected care, technology-enabled care, clinical decision making, engagement with payment models, and advocacy. (McGivney)
- A scaffolded pedagogy helps ensure that learners move toward being practice ready, and short courses or certificate programs can teach practicing pharmacists about new areas, such as pharmacogenomics, informatics, and implementation science. (Smith)
- Pharmaceutical industry demand for Pharm.D.s will continue to rise over the next 5–10 years. (Alfonso-Cristancho)
__________________
*These points were made by the individual workshop speakers/participants identified above. They are not intended to reflect a consensus among workshop participants.
In his opening remarks, Watanabe described how the Next Generation Education and Training Programs session was designed with a broad, education-to-practice perspective in mind. The aim of the session is to show how pharmacy education has evolved and adapted to new learning and practice environments, he reflected, and how future graduates can be trained to lead and promote a forward-looking workforce within constantly evolving education and practice environments. Leigh Ann Ross, Auburn University, moderated the session.
“I come from a family of pharmacists,” said Ross, before describing a picture of her dad showing him compounding in his pharmacy many years ago. She then wondered out loud whether that pharmacist could have predicted where pharmacy would be today—delivering 90 percent of the vaccines during a pandemic, managing complicated medication regimens, and providing patient care. It is hard to imagine how the next 40 years of pharmacy will evolve, she said, but what is known is that the environment will continue to be reshaped by forces such as digital health policy changes, chronic disease complexity, and public health needs. The question is not just how pharmacy education should respond but how it and educators can proactively shape the future of pharmacy. What are the skills and mindsets that future pharmacists will need, she asked, and how do the field and all of its stakeholders ensure that education and training systems can keep pace? This session, said Ross, would explore the past evolution of pharmacy, current landscape, and future. A panel of speakers shared their vision of pharmacists as clinicians, innovators, leaders, and policy influencers. Ross encouraged participants to consider what type of pharmacist communities will be needed in 40 years and how learners of today can be prepared for this future.
EVOLUTION OF PHARMACY EDUCATION AND TRAINING
The profession has made significant advances over the past 50 years, said Joseph T. DiPiro, Virginia Commonwealth University. These changes include funding from universities for early clinical pharmacists; expanding scope of practice for more patient-focused (clinical) services; converting practice requirements from a B.S.Pharm. to a Pharm.D.; sustaining residencies and fellowships; establishing board certification; and developing the Pharmacist Practice Model Initiative, Pharmacists’ Patient Care Process, and Curricular Outcomes and Entrustable Professional Activities. In essence, pharmacy has changed more than perhaps any other health profession, he said. Past education and training programs did not include a focus on many issues that are now relevant to practice; education programs largely did not focus on patient care, professionalism and leadership, practice models, cultural learning, understanding of payment models, health disparities and social determinants of health, and technology training. However, said DiPiro, certain aspects of past education were and remain critical. Pharmacy has always had a strong foundation in the sciences and an emphasis on postgraduate training and lifelong learning. Pharmacists have shown a willingness to change and enhance their education and training aimed at improving care and developing the profession for the good of the public. Throughout all the changes, pharmacists have always been seen as trusted health professionals.
While pharmacy has changed greatly over the years, DiPiro underscored the importance of continuing to adapt and evolve the profession due to several current factors. Patients continue to have medication issues, with concerns about access to medicines and consumer costs. The aging population and demographic changes have led to a high prevalence of chronic disease. Payment models and the national and state expenditures on medication raise challenges. Technology and artificial intelligence (AI) are shifting workplace and practice models, and pharmacist burnout is a major challenge that needs attention. Pharmacists are directly connected to all of these issues and can make a positive impact on the health of patients, communities, and the country.
CURRENT LANDSCAPE OF PHARMACY EDUCATION AND TRAINING
The pandemic changed the public perception of pharmacy, said Melissa Somma McGivney, University of Pittsburgh. In particular, it changed what potential students and their families think of it. McGivney said that she has always asked first-year pharmacy students whether they have ever worked with a pharmacist on something other than getting a medication. Postpandemic, nearly every student raised their hand. People’s experiences with community pharmacy are powerful, she said, and the “front door” to the profession. The public has seen pharmacists administer vaccines, test and treat, and prescribe medication for minor ailments and conditions. Communities have experienced pharmacist management of high-specialty medications and treatments, in both managed care and bedside-to-home contexts and pharmacists working with technology to improve medication use and patient care. Despite a new perception of pharmacists and their services, said McGivney, their ability to provide services varies widely by state. In some states, they can test and treat conditions such as COVID-19, flu, and strep and furnish medications for opioid use disorder, HIV prophylaxis, and hormonal contraception. This variation among states can be confusing for students and faculty, because of the different requirements for graduation. Another challenge for students, she said, is the reality of community pharmacies closing across the country; this is making students “question where they want to be.” Despite these challenges, students are looking to be inspired, said McGivney. They want to make a difference, care for those around them, and grow in the profession.
The Accreditation Council for Pharmacy Education (ACPE) set new standards in 2024 that take effect in 2025 and reflect some of the changes occurring in pharmacy and what pharmacists will be expected to know and do in the future. McGivney highlighted six particular additions or changes to the required elements in the Pharm.D. curriculum: health care systems
payment models, the history of pharmacist-provided patient care, laws and regulations, physical assessment and screenings, diagnosing and prescribing, and advancing public health and wellness. These standards, she said, are challenging schools of pharmacy to do things differently.
The responsibility for shaping the future of pharmacy is shared between education and practice, said McGivney. Educators have a responsibility to recruit new pharmacists, follow ACPE standards, guide their students through experiential rotations and assess their competence, adapt to the post-COVID-19 world, and help students with postgraduation employment. Practitioners’ responsibilities include transitioning the practice model, taking on expanded roles, and addressing challenges with payment for service and access to care. Partnerships between academia and practice are essential for creating transformative opportunities and innovation.
Students are ready to be leaders and change agents, said McGivney. To facilitate student leadership, “they need to experience the future of pharmacy now,” she said, so they are prepared and inspired to guide the future. This means exposing learners to high-quality interprofessional practice, community-connected care, technology-enabled care, clinical decision making, engagement with payment models, and advocacy. McGivney encouraged current pharmacists to work together with the pharmacists of the future and remove silos between different types of pharmacy. “We are all pharmacists,” she stressed, and “we are in this together.”
FUTURE OF PHARMACY
Speakers addressed specific topics on the future of pharmacy: licensure standardization, adaptable education and training, innovative education, and evolving roles for Pharm.Ds.
Licensure Standardization
Recent years have seen an uptick in the percentage of pharmacy graduates who are not getting licensed, said Lemrey “Al” Carter, National Association of Boards of Pharmacy. In some states, graduates have a certain number of years to become licensed; after that, they must take additional coursework. Carter noted a need to investigate why graduates are opting out of the North American Pharmacist Licensure Examination exam and create strategies to encourage them to pursue licensure regardless of their immediate career plans. The Multistate Pharmacy Jurisprudence Examination (MPJE), which tests knowledge of pharmacy laws and regulations, is also required for licensure in nearly every state. However, he said, it is not standardized across states, and these gaps can lead to variability in public safety protections. Pharmacists seeking licensure in multiple states must sit
for and pass multiple MPJEs, which can make it more difficult for qualified pharmacists. Carter said that most state-specific laws are similar, if not identical, so it should be possible to develop a more standardized, uniform approach.
The National Association of Boards of Pharmacy (NABP) is creating a uniform MPJE, said Carter. A steering committee has been working since 2023, with a review committee recruited in 2024. It created an exam blueprint and content outline and has been moving toward developing and testing its questions. Carter shared four areas that are similar across all states:
- Pharmacy and pharmacist practice (e.g., scope of authority/practice, adulterated or misbranded medications, federal regulatory standards),
- Medication use process (e.g., prescribing, transcribing and documenting, dispensing, administering, and monitoring),
- Regulatory authority and legal obligations (e.g., role of regulatory authorities, controlled substances, liability), and
- Pharmacy operations (e.g., personnel and facility, recordkeeping).
The uniform MPJE is envisioned as an additional resource for boards, he said, rather than a sole mandate. It is not a federal law exam; rather, it is designed to assess knowledge of “universal” state laws and regulations to ensure competency and protect public health and safety. Carter stressed that candidates can still be held accountable by the state boards of pharmacy and subject to disciplinary action if they do not follow state-specific laws. The test is set to launch in June 2026; Carter said the next challenge will be getting states to adopt it. States that recognize it will have the capability for license portability. He further noted how the new model of pharmacy practice means that people are not always practicing in one state; rather, they may be crossing state lines to reach rural or underserved patients and providing virtual care. To obtain an interstate privilege, a pharmacist would need to hold a license in their resident state, comply with its continuing education requirements, pass a state or uniform law exam, pay fees and submit to background checks, and practice within the laws and regulations of the other state.
License portability is the first step in a standardized approach for licensure, said Carter. Future efforts will focus on a standard-of-care model across all states, payer recognition for pharmacists, and a national pharmacist licensure examination. With the demand for pharmacists growing and the model of services evolving, a standardized approach would ensure that pharmacists can work in the communities that need them.
Adaptable Education and Training
“We live in a VUCA world,” said Marie Smith, University of Connecticut. She explained that VUCA stands for volatility, uncertainty, complexity, and ambiguity. Over the last 100 years, the profession of pharmacy has thrived—not just survived—through many similar difficult times. It has evolved, health care payment systems have changed, and the health care delivery ecosystem has transformed. Pharmacists have “lived through a lot of VUCA moments in our practice lifetimes,” she said. For future pharmacists to continue to be able to adapt and transform practice as the world changes, they would need the requisite education and training to do so, and Smith identified several key components:
- Foundational sciences and “pharmaco-everything”;
- Leadership skills, adaptability, and resilience;
- Critical-thinking and change management skills;
- Implementation science;
- Interprofessional experiences—virtual or in person;
- Simulations: electronic health records, health information exchange, patient assessment, care plans;
- Health services research: expanded workforce/pharmacist roles with payment reform; and
- Value of impact (VOI) based on quintuple aim dimensions.
Smith explained that she prefers VOI rather than return on investment (ROI). Pharmacists bring tremendous value to the health care system, but it cannot always be measured and explained in terms of ROI. For example, it is estimated that one full-time primary care pharmacist providing comprehensive medication management (CMM) services can open up around 1,900 patient appointments for the primary care provider each year (Smith, 2025). This is equivalent to about 35 appointments a week, she said, which is a tremendous value, for both patient access to care and provider well-being.
In addition to focusing on education and training during the early years of a pharmacist’s career, Smith called for shifting to a culture of lifelong learning. This means emphasizing connecting knowledge, decision-making skills, and action plans rather than “binging and purging” information for exams. A scaffolded pedagogy helps ensure that learners move toward being practice ready, and short courses or certificate programs can teach practicing pharmacists about new areas, such as pharmacogenomics, informatics, and implementation science, she said.
Smith introduced participants to Kotter’s Change Management Model (see Figure 5-1). This model, she explained, is useful for guiding a change process at a system, organization, group, or individual level. She urged
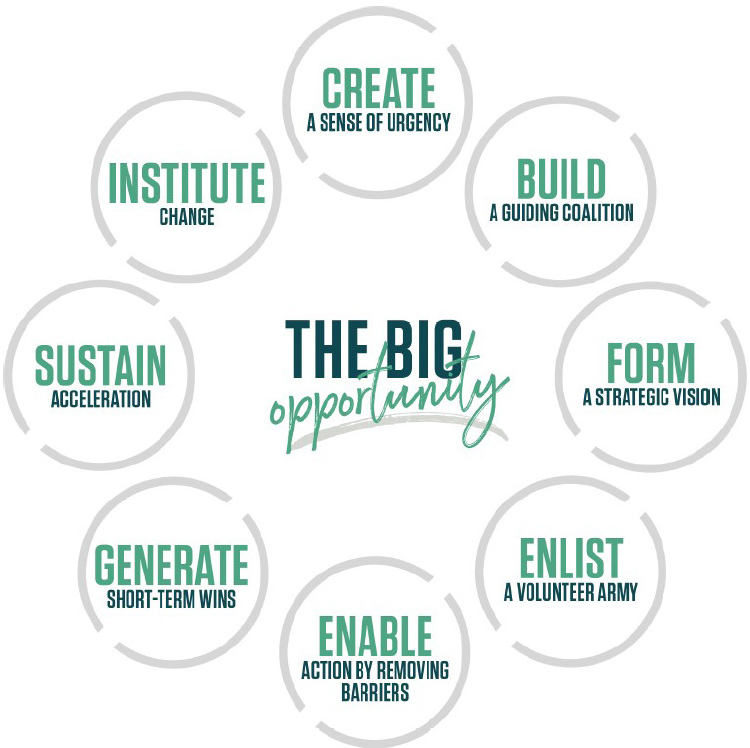
SOURCE: Presented by Marie Smith on May 30, 2025. Used with permission from Kotter International Inc. (n.d.)
stakeholders who want to make changes to the profession to consider where on the “clock” they are. Smith noted that people tend to skip very important steps, which leads to a higher likelihood of failure. The design-thinking framework is another method for implementing change; it includes defining the challenge, identifying the main problem, brainstorming, creating solutions, and refining and reiterating.
Smith closed by calling on educators to consider bringing back the requirement for capstone projects in Pharm.D. programs. These develop a huge number of skills, she said, including critical-thinking, project management, teamwork, interdisciplinary communications, technical writing, and
presentation skills. Requiring a capstone project gives students an opportunity to develop these skills early in their career—which they will take with them as they move through their pharmacy practice and the changing world around it.
Innovations in Education, Training, and Practice
It is difficult to predict the future, said Samuel Johnson, the Craneware Group. The rapid development and integration of technologies such as digital health tools and AI sometimes feels like a “choose your own adventure book.” He explained that multiple paths could lie ahead and that it is critical that stakeholders be circumspect and thoughtful about how technologies are implemented. It is urgent that stakeholders think through how to use technology to our benefit and implement systems and policies that direct us down a better path. He gave the example of a moving sidewalk at the airport; some stand on the sidewalk and get carried, while others walk on it and get where they’re going much faster. Johnson emphasized the importance of working with technology to improve performance, rather than letting it take over “everything.”
As technologies are integrated into the health care system, said Johnson, it will be important to ensure that vital protections—such as patient privacy—are maintained and strengthened. In addition, everyone involved in pharmacy education and practice would be wise to stay informed about evolving regulations that govern the use of technology in health care, to ensure compliance. This would mean continuously adapting training to keep pace with advancements and effectively integrating them into practice, he said. Johnson offered some ideas of how he envisions the profession evolving in education, practice, and workforce development:
- Education: Schools will adopt simulation labs and virtual reality for hands-on training, enhancing clinical skills in a controlled environment.
- Interprofessional education: Educators will emphasize interdisciplinary training to prepare pharmacists for collaborative relationships with other health care professionals.
- Clinical Services: Pharmacists will play a larger role in chronic disease management, preventive care, and precision medicine.
- Public Health: Community pharmacists will be further involved in community health initiatives, vaccination programs, and health education.
- Continuous Professional Development: Pharmacists will engage in ongoing education and training to keep pace with technological advancements and evolving health care needs.
- Recruitment and Retention: Pharmaceutical organizations will create strategies to attract and retain skilled pharmacists by offering incentives to enrich career growth opportunities.
The youth of our country—that is, potential future pharmacists—think differently, said Johnson. They have grown up with technology and are used to solving problems that seem difficult to others. He joked that his twin 14-year-old sons demonstrate this aptitude when getting around the restrictions on their cell phones. “Let’s put that energy to good use,” he said, and be thoughtful about how technology is implemented and integrated into health care. Certain challenges are usually seen as headwinds to progress, such as burnout, economic pressures, and regulatory changes. Approaching these issues and moving toward the future thoughtfully, he noted, can transform these from headwinds into tailwinds.
Evolving Roles for Pharm.D.s
Pharm.D. graduates have many potential career paths, said Rafael Alfonso-Cristancho, GlaxoSmithKline. About 25 percent pursue a nontraditional career, such as in the pharmaceutical industry, where they usually work in one of three areas: research and development, medical affairs and compliance, and health economics and outcomes research. The demand for them is driven by a variety of factors, particularly the increase in Food and Drug Administration (FDA) precision medicine approvals and AI-/data-related productivity boost in research and development. Demand is increasing, said Alfonso-Cristancho, but is academia responding by increasing the supply of industry-ready graduates? About 60 percent of pharmacy schools offer industry-related training and/or dual degrees in Pharm.D. and business or other areas, with a 35 percent rise in industry fellowships. Alfonso-Cristancho said that fellowships are very valuable for both the learner and the industry because they allow the learner to understand what the work is and whether it fits their expectations and the company to provide on-the-job training and identify knowledge or skill gaps. Bringing Pharm.D.s into the industry does have challenges, he said. The training and skills may be different from those needed for a traditional clinical path, and shifting from a clinical to industry mindset requires adaptation. Furthermore, not everyone in industry understands the value proposition of Pharm.D.s and the unique skills they can bring.
Alfonso-Cristancho commented that pharmaceutical industry demand for Pharm.D.s will continue to rise over the next 5–10 years. They will lead personalized therapy initiatives and AI-driven drug development, and their expertise in digital therapeutics and real-world data analysis will become critical. He predicted that they will be in multiple leadership roles
in industry, including C-suite positions in major biopharmaceutical companies. He emphasized that one of their most important contributions will be their perspectives on what is valuable for patients and how to keep patients at the center when developing medicines. Bringing a drug to market does not equal success, he said; a drug is only successful and effective if patients take it and stick with it. Pharm.D.s are essential to the future of the biopharmaceutical industry, said Alfonso-Cristancho. Both educators and students need to be open to evolving, nontraditional career paths. “Your Pharm.D. can change the world—not just treat it,” he concluded.
DISCUSSION
Ross facilitated a discussion among the presenters. She began by asking the panelists to identify specific examples of innovative approaches for NextGen education and training. DiPiro shared his experiences at Virginia Commonwealth University. The first step, he said, was to define “NextGen pharmacy.” DiPiro and his colleagues started a consensus-building process in 2019 to think about what was needed and how the curriculum needed to be changed to be relevant for the future. He noted that while his group did not call this process “design thinking,” they did follow many of the same steps described by Smith. After agreeing on a definition, their next steps were to conduct a careful analysis of the current and possible future roles of pharmacists and identify what kind of knowledge and skills would be needed. This information was used to inform the curriculum and develop competencies and courses that matched with these roles. DiPiro said they had external input at multiple stages, particularly from employers. While the pandemic delayed the process, the new curriculum is now being implemented. DiPiro further reflected on the development process saying they used Kotter’s Change Management Model (see Figure 5-1) to guide their multilevel discussions and spent a lot of time at the start discussing why the change was even needed. If others outside of their group did not buy in to the sense of urgency, he said, they would be less likely to get on board. DiPiro commented on two key challenges they dealt with during development: making space for new content in the curriculum and implementing a mechanism for continual updates for flexibility and adaptability.
McGivney shared her experiences at the University of Pittsburgh. It has eight “areas of concentration” (University of Pittsburgh School of Pharmacy, n. d.), which allows students to personalize their education. Roughly half of pharmacy students go on to postgraduate training; the other half go directly into the workforce. Despite a lot of postgraduate opportunities, she said, the pharmacy program wants to capitalize on the time students are in school. Within these areas, students have a group of faculty that serve as mentors. This becomes a “place of belonging” within the school, said
McGivney. Each area has a project that students must complete. While this program does not necessarily change where students land after school, she said, it makes them ready for leadership when they graduate.
Alfonso-Cristancho identified gamification as an innovative approach that he has seen. Giving students a challenge, along with rules and opportunities for solving it, allows them to think creatively and develop innovative solutions. For example, he said, a project in Brazil brought together students of data science, pharmacy, and medicine to solve a problem about respiratory conditions. They were given public datasets and asked to develop data visualizations to demonstrate what the priority issues should be. Alfonso-Cristancho commented on how amazed he was at the number of insights they brought to the challenge and that their research—which took them several weeks to complete—would have otherwise taken years and hundreds of thousands of dollars. Students have a lot of experience with technology and learn differently than in the past; Alfonso-Cristancho urged educators to identify and leverage student assets and use innovative approaches that bring out valuable skillsets of their current students.
Johnson shared details about his experience as a visiting scholar with the American Board of Family Medicine. He said it was “illuminating” for two reasons. First, the interprofessional collaboration became a springboard for professional development and advancement and gave him far greater insight into the challenges and opportunities in the broader world of health care. In light of the statistics about the primary care shortage and pharmacy deserts, Johnson noted a gap in providing sufficient opportunities for pharmacists, primary care providers, and other health care professionals to collaborate. The second insight was that the board conducts a great deal of research with its members and collects data that inform its advocacy strategies. Johnson suggested that pharmacy organizations could build more infrastructure to consistently and comprehensively track the value and impact of pharmacy practice. While there are data from pilot projects, it would be advantageous to set up a continuously evolving dataset to validate the work of pharmacists in multiple settings, he said.
Other Areas of Discussion
Jennifer Bacci, University of Washington School of Pharmacy, facilitated a question-and-answer session, inviting questions and comments from participants, on such areas as
- Emphasizing the importance of teaching and prioritizing advocacy and policy in the curriculum for all health professionals (Jeff Wrapper);
- Using a scaffolded approach to develop foundational knowledge and building on it with advanced training or electives (Smith);
- Effectuating a desire for more coordination between academia and practice, specifically in terms of residency training programs and giving graduates opportunities to use their skills and knowledge (DiPiro, McGivney);
- Strategically planning community pharmacy residency programs to address pharmacy deserts, financial sustainability, and other challenges (McGivney);
- Employing greater flexibility in pharmacy programs that could allow students to pursue nontraditional areas of concentration (McGivney, DiPiro);
- Promoting dual-degree programs to leverage efficiencies and increase the number of pharmacists with expertise beyond pharmacy (DiPiro, Smith);
- Increasing pharmacy students’ exposure to different areas of practice within the field (McGivney);
- Adapting curricular design to be aligned with advancements in AI while also leveraging AI to maximize unique learning situations (Johnson, Carter);
- Creating opportunities for pharmacy students and practitioners to develop and practice leadership skills and promote the stories of pharmacists that go beyond statistical data points (DiPiro, McGivney, Chisholm-Burns);
- Preparing students to serve in multiple roles, while ensuring they develop the basic knowledge and skills of clinical pharmacy (Alfonso-Cristancho, Johnson);
- Investing in education and training to produce high-quality technicians who can contribute to the vision for the future of pharmacy (Sean Kim, Carter);
- Leveraging competency-based education to fill gaps across the continuum of growth for pharmacists and ensure that they are practice ready at graduation and continuously learning throughout the rest of their careers (Denise Rhoney [participant], McGivney); and
- Integrating a focus on mental health and well-being so students and practitioners are better equipped to adapt to an ever-changing environment that can be a root cause of stress and burnout (Alex Varkey [participant]).











